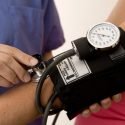
Hypoglycemia Symptoms and Treatments
What is Hypoglycemia? What are the Symptoms of hypoglycemic reaction or low blood sugar levels, and what should you do if you experience them?
Hypoglycemia is a condition in which the blood sugar levels are too low. Symptoms, causes, and natural treatments for hypoglycemia are discussed in this article.
One of the most frequent health issues globally is uncontrolled glucose levels. Symptoms of hypoglycemia are common in individuals with prediabetes or diabetes, but they’re also connected to other health issues, including high blood pressure, high cholesterol, and even arthritis. Unfortunately, hypoglycemia has been considered “an under-appreciated condition” that is the most prevalent and significant adverse effect of glucose-lowering diabetic medicines, even though it is seldom acknowledged.
Persons who are sick, overweight, or sedentary are at risk for both hypoglycemia and hyperglycemia; anybody who eats a bad diet and has problems with normal glucose metabolism might develop symptoms. Hypoglycemia and associated disorders are exacerbated by the traditional American diet, which is heavy in refined carbohydrates and sugar but poor in nutrients like healthy fats and fiber.
What are some signs that you may be suffering from hypoglycemia symptoms, and what can you do to control them?
Hypoglycemia symptoms include sudden hunger, irritation, headaches, cognitive fog, and shakiness, which are sometimes misdiagnosed as other illnesses. You may help manage low blood sugar symptoms and prevent them from reoccurring by reducing your consumption of empty calories, changing your nutrition, and paying attention to how mealtime and activity impact you.
What Is Hypoglycemia?
Hypoglycemia, commonly known as low glucose, is a disorder characterized by low blood sugar levels. Glucose is mostly found in carbohydrate and sugar-containing diets, and it is one of the body’s most essential sources of energy.
Here’s a quick rundown of how glucose works after it enters the body, as well as how our hormones control blood sugar levels:
- Glucose is taken into the circulation from meals containing glucose (such as fruit, vegetables, legumes, grains, and sweet snacks) and then delivered throughout the body to cells for energy.
- The hormone insulin, which is produced by the pancreas in response to how much glucose we ingest, is required for our cells to utilize glucose.
- Insulin aids in absorbing the glucose our cells need for energy, with any excess glucose being transported to the liver or other muscle tissues to be stored as glycogen for later use.
- We can build fat cells (which form adipose tissue or body fat) from surplus glucose that we don’t need for energy and store glycogen as an energy store that may be accessed when required.
- When blood glucose levels fall too low in healthy adults, the hormone glucagon signals the liver to release stored glycogen to maintain a healthy blood glucose level.
- Blood sugar levels stay low, and hypoglycemia symptoms arise if this process is disrupted for any reason.
Hyperglycemia is the condition produced by excessive blood sugar and is the polar opposite of hypoglycemia (high glucose). If a person’s diabetes or prediabetes isn’t well-controlled, hyperglycemia is a frequent complication. Hyperglycemia produces diabetes-related symptoms such as thirst, urination, exhaustion, and dizziness.
People with diabetes may also get hypoglycemia if their blood sugar levels fluctuate dramatically owing to insulin and glucose mismanagement. Hypoglycemia is a dangerously adverse effect of blood-sugar-lowering drugs (including insulin) that cause glucose levels to decrease too quickly or from not eating a balanced, nutritious diet in patients with diabetes. In addition, research has shown that repeated bouts of hypoglycemia may weaken a person’s defensive systems against low blood sugar, leading to serious problems such as a sixfold increase in the chance of dying after a severe episode.
Symptoms and Signs
Have you ever felt jittery, irritable, or exhausted immediately before a meal? Have you ever gone on a diet and purposely missed meals, only wanting sweets and feeling exhausted? You’ve probably felt what it’s like to have low blood sugar.
The following are the most frequent hypoglycemia symptoms or indicators of low blood sugar:
- Hunger, which may be severe and abrupt at times
- Anxiety symptoms
- Sweating, especially night sweats (a symptom of “nocturnal hypoglycemia”).
- Feeling light-headed or dizzy
- Experiencing lethargy, tiredness, or grogginess
- Having difficulty sleeping and waking up tired
- Having mood swings and being grumpy
- Paleness of the skin of the face
- Headaches
- Muscle deterioration
- Feeling confused and having problems functioning or focusing are brain fog symptoms.
- Seizures, unconsciousness, and even death may occur in extreme situations (particularly when diabetic medicines are involved). Diabetic people are the most vulnerable to severe hypoglycemia episodes, particularly if they often occur over time. Severe hypoglycemia episodes have been linked to an increased risk of dementia, heart disease, functional brain failure, nerve damage, and mortality in elderly diabetic patients.
When blood sugar levels aren’t controlled, it’s possible to have symptoms of both hyperglycemia and hypoglycemia. In addition, over time, they might lead to issues and side effects suggestive of prediabetes or diabetes, such as tiredness, sugar cravings, blood pressure abnormalities, weight loss or increase, nerve damage, and anxiousness name a few.
Causes and Risk Factors
What are the fundamental causes of hypoglycemia symptoms in people? Hypoglycemia may be caused by a variety of factors, including:
1. Insulin Mismanagement
When too much sugar is in the blood, insulin levels increase and fall, eventually leading to insulin resistance (when cells stop responding to normal amounts of insulin). This may lead to diabetes or other metabolic syndrome symptoms in some people, but it can also cause blood sugar levels to fluctuate in people who don’t have diabetes.
2. Poor Diet
Hypoglycemia may be caused by eating too little food, going without meals for lengthy periods, or having vitamin deficiencies. Diets that entail eating short meals or skipping meals entirely, such as fads or crash dieting, may also create symptoms. However, in certain investigations, insufficient meal intake was identified as the No. 1 most prevalent cause of severe hypoglycemia episodes. This is referred to as “impaired counter-regulatory systems,” and it basically implies that failing to notice your own hunger signals might lead to severe hypoglycemia symptoms.
3. Medications for Diabetes
People with diabetes are often treated with drugs to counteract their resistance to insulin’s typical actions or to reduce high blood sugar levels. Clinical research has indicated that attempting to reach aggressive healthy blood sugar levels with insulin and glucose medicines is linked to a threefold increase in the incidence of hypoglycemic symptoms. According to the Indian Journal of Endocrinology and Metabolism, this hypoglycemia impact is now widely seen as a major issue, even “counterbalancing the advantages of rigorous glucose management.” Chlorpropamide (Diabinese), glimepiride (Amaryl), glipizide (Glucotrol, Glucotrol XL), repaglinide (Prandin), sitagliptin (Januvia), and metformin are all medications that might cause hypoglycemia.
4. Medications for Treating Other Illnesses
When some drugs are taken with insulin, blood sugar levels might be dangerously low. Pramlintide (Symlin) and exenatide are two of them (Byetta).
5. Increased Physical Activity
Low blood sugar may be caused by over-exercising, overtraining, and not eating afterward. Muscles heal themselves by using glucose from the blood or stored glycogen, so it’s critical to refuel after an exercise to avoid discomfort.
6. Other Medical issues
Hormone imbalances, autoimmune illnesses, eating disorders, organ failure, and cancers that influence hormone levels may all impact insulin release, glucose uptake, and glycogen storage.
7. Alcohol
Alcohol boosts blood sugar levels, but they might drop too low later.
8. Deficiencies in enzymes
Certain metabolic conditions might make it difficult for the body to break down glucose adequately or for the liver to release glycogen when it is required.
9. High-Stress Levels
Cortisol levels may rise due to stress, interfering with how insulin is utilized.
Conventional Treatment
Conventional hypoglycemia therapies, according to the American Diabetes Association, are as follows:
- Making dietary and lifestyle modifications to improve blood glucose management. Changing meal frequency or following a diabetic diet plan are examples of this.
- When hypoglycemia symptoms first appear, doctors frequently advise taking 15–20 grams of glucose (from carbs) very quickly.
- Keep an eye on your symptoms for around 15 minutes, and check your blood sugar if you have diabetes.
- To avoid recurrence of symptoms, eat a small snack every two to three hours. At least 15 grams of carbs should be included in snacks and meals.
- To manage hypoglycemia symptoms in diabetic patients, doctors may give drugs such as glucose pills or gel and other medications. In addition, injectable glucagon kits are sometimes used to treat people with diabetes who have gone unconscious due to severe insulin response.
Natural Treatments
1. Adhere to a Hypoglycemic Diet
If you’ve experienced hypoglycemia before, consider following a balanced diet plan and keeping note of your symptoms to figure out how to get your blood sugar levels back to normal.
Hypoglycemia symptoms may be managed with the following foods:
- Artichokes, green leafy vegetables, chia seeds, flaxseeds, beans, apples, pumpkin seeds, almonds, avocado, and sweet potatoes are all high-fiber foods to consider.
- Carbohydrates are the primary source of glucose in the diet; however, not all carbohydrates are created equal. Brown or wild rice, sweet potatoes, sprouted ancient grains, lentils, and beans are all good options.
- Fruit and fresh fruit juice and vegetables, and entire pieces of fruit may assist in counteracting a hypoglycemic episode.
- Virgin coconut oil, MCT oil, extra virgin olive oil, nuts and seeds (almonds, chia, hemp, flax, for example), and avocado are all rich sources of healthy fats.
- Quality protein sources include wild fish like salmon, free-range eggs, grass-fed cattle or lamb, raw dairy products (such yogurt, kefir, or raw cheeses), and pasture-raised fowl.
The following foods should be avoided:
- Caffeine or alcohol abuse
- Empty calories, such as those found in highly processed packaged foods
- Added sugar in abundance
- Drinks with added sugar
- Grain that has been refined
- Fried foods and fast food
2. Think twice about skipping meals or restricting your calorie intake.
People with hypoglycemia or diabetes should have frequent meals throughout the day, consume sufficient calories at each meal (typically containing at least some healthy carbs), and never skip meals. Healthy snacks every several hours may also help maintain blood sugar levels constant and avoid energy dips.
If you’re exercising and feeling weak or dizzy, make sure you’re getting enough nutrition, take a break, and try taking a small snack before you start. After an exercise, refuel with a snack high in protein and low in bad carbohydrates. If you detect signs of hypoglycemia while sleeping, try eating a snack before going to bed to avoid hypoglycemia overnight.
3. Discuss your medications with your doctor.
If you’re taking any drugs that affect blood glucose or insulin levels, keep a close eye on any physical signs or symptoms that might indicate hypoglycemia. According to research, hypoglycemia symptoms might grow less strong over time or perhaps disappear entirely, resulting in “hypoglycemia unawareness” in a considerable percentage of patients who have had many episodes owing to drugs. Consult your doctor about how you can better manage your blood sugar levels and if your dose should be adjusted to alleviate symptoms.
The Facts
- The most common cause of hypoglycemia episodes is calorie restriction (via dieting, fasting, or missing meals). Other significant reasons include excessive activity without enough replenishment and insulin usage at dangerously high levels.
- Insulin medicines may sometimes cause severe hypoglycemia, even fatal hypoglycemia. According to various studies, severe hypoglycemia affects 35 percent to 42 percent of diabetes patients on insulin, and the average incidence of severe hypoglycemia attacks throughout the course of a patient’s lifetime is 90–130 episodes.
- According to studies, the longer someone has diabetes (for example, over 15 years), the greater their likelihood of experiencing severe hypoglycemia symptoms on several occasions.
- The risk of mortality in type 1 diabetes patients who have not been diagnosed or treated is much greater than in healthy people. For example, in young persons with type 1 diabetes, nocturnal hypoglycemia is responsible for 5% to 6% of all fatalities.
- The number of emergency room visits due to hypoglycemia in the United States is estimated to be about 298,000 per year.
- Most individuals should eat every three to four hours to help avoid hypoglycemic symptoms, and every meal should include at least 15 grams of carbohydrates.
Blood Sugar Chart for Hypoglycemia
Are you curious about what blood glucose levels are regarded to be too high or too low? Experts generally believe that there are no apparent distinctions between the normal blood sugar range and the high and low blood sugar levels. Researchers and clinicians, on the other hand, often utilize the blood sugar chart below to classify various conditions:
Blood Sugar Levels That Are Normal
Healthy blood sugar levels are regarded to be between 60 to 140 milligrams of sugar per deciliter of blood (mg/dL). However, there is a typical “range” since even perfectly healthy people’s blood sugar levels fluctuate throughout the day depending on how they eat and how active they are. Healthy blood glucose levels are measured in millimoles per liter (mmol/L), which is an international unit.
It’s typical for blood sugar to be between 70–99 mg/dL (less than 100 mg/dL) if you’re usually healthy (you don’t have diabetes) and haven’t eaten anything in the last eight hours (you’ve been “fasting”).
It’s typical for blood sugar to be less than 140 mg/dL if you’re healthy and haven’t eaten in the last two hours.
Hypoglycemia
Anything below 60–70 mg/dL is usually considered low. If you have a history of diabetes, your fasting glucose level should be less than 100 mg/dL, which may need the usage of insulin. Prior to eating, blood sugar levels of 70–130 are also considered good. If you have diabetes, your blood sugar should be between 100 and 140 mg/dL before going to bed and at least 100 mg/dL before exercising.
Hyperglycemia
If type 1 diabetes is not treated, blood glucose levels may reach 500 mg/dL (27.8 mmol/L) at times. People with type 2 diabetes are less likely to have blood sugar levels this high, particularly if they take medicines or maintain a healthy lifestyle. For example, if you have diabetes and have eaten in the last two hours, your blood sugar should remain below 180 mg/dL.
Precautions
If you experience severe and abrupt indications of hypoglycemia, such as fainting, see a doctor or go to the emergency department. Tell your doctor right away if you ever pass out or have a seizure while taking drugs that may affect your blood glucose.
If you have diabetes, it’s a good idea to train someone how to use glucagon to treat severe hypoglycemia and to have that person phone 911 immediately away if there’s an emergency. Don’t overlook dangerous indicators that persist over time, such as passing out, sleeplessness, fast heartbeats, and so on, since this increases the chance of long-term consequences.
Final Thoughts
- Hypoglycemia is a condition in which blood glucose (blood sugar) levels are unusually low.
- Hunger pains, shakiness, anger, dizziness, and exhaustion, are all common hypoglycemia symptoms.
- Cutting calories, skipping meals, a poor diet, vitamin deficiencies, and not eating after exercise are all causes of hypoglycemia.
- Severe hypoglycemia symptoms, also known as insulin response or insulin shock, are particularly common in patients with diabetes who use medicines.
- Natural hypoglycemia remedies include eating every few hours, eating a balanced meal, recharging after activity, and avoiding using drugs that interfere with blood sugar management too often.
FDA Compliance
The information on this website has not been evaluated by the Food & Drug Administration or any other medical body. We do not aim to diagnose, treat, cure or prevent any illness or disease. Information is shared for educational purposes only. You must consult your doctor before acting on any content on this website, especially if you are pregnant, nursing, taking medication, or have a medical condition.
HOW WOULD YOU RATE THIS ARTICLE?